It is estimated that 1.1 million people in the United States are infected with HIV. Of those, 1 in 7 do not know they are infected.[1] The number of new HIV diagnoses fell 19% from 2005 to 2014.[1] Because HIV testing rates have remained stable or increased in recent years, this decrease in diagnoses suggests a true decline in new infections. The statistics in the Southern United States are not as promising. In 2015, the South accounted for 52% of the 18,303 new AIDS diagnoses in the United States, followed by the Northeast with 18%, the West 17%, and the Midwest with 12%.[1] In 2015, the rate of new AIDS diagnoses was 7.9 in the South, 5.9 in the Northeast, 4.1 in the West, and 3.4 in the Midwest.[1] Of the 6,721 deaths attributed directly to HIV or AIDS in 2014, 53% were in the South, 19% were in the Northeast, 17% were in the West, and 11% were in the Midwest. [1]
The statistics for Florida are more alarming, with that state ranked 1st among the 50 states in the number of HIV diagnoses in 2015.[2] This year the number of reported HIV cases in Florida has jumped 23 percent, the biggest increase in a continuing upward trend that began in 2012 after several years of decrease. The proportion of Floridians infected with HIV is at its highest level in 7 years.[3] Increases in new infections are present in almost every county of the state. A review of all counties in Florida shows that the highest rates of new infections are in Miami-Dade County with 47%, followed by Broward with 41.5%, Orange with 35.5%, and Hillsborough with 30%.[4]
For the dental profession, the state statistics are of particular importance. In the absence of antiretroviral therapy (ART), oral manifestations are the earliest significant indicators of HIV infection.[5] Oral lesions are common (30–80%) in patients infected by the HIV virus and may indicate an impairment in the patient's general health status.[6]
Clinical and epidemiological observations have shown a considerable decline in the morbidity of people with HIV since new advancements in ARV treatment were made in the late 1990s. There has been a significant shift in both the type and frequency of oral lesions seen in people with HIV. Patients on ART show a lower incidence of oral lesions including candidiasis, oral hairy leukoplakia, and Kaposi sarcoma.[7] The prevalence of oral lesions has decreased by more than 30% since the late 1990s.[8]
However, there has been an increase in prevalence of caries and periodontal disease. This increase most likely can be attributed to significant findings of xerostomia in people with HIV. Xerostomia is the subjective complaint of oral dryness. This must be distinguished from salivary gland dysfunction which is an objective disease characterized by reduced salivary flow. Studies have shown that 40% or more of people with HIV experience major xerostomia during their disease course. Studies of people with HIV with xerostomia show a frequently negative effect on their quality of life.[9]
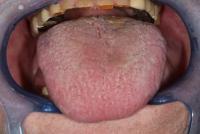
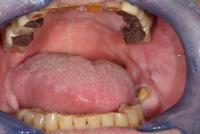
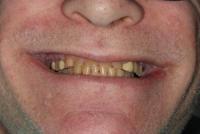
Symptoms of xerostomia include cracked or peeled atrophic lips, glossitis (Figure 1), and pale dry buccal mucosa (Figure 2). Xerostomia can lead to dysphagia, dysgeusia, oral pain of unknown origin, dental caries, oral infections, periodontal disease, and angular cheilitis associated with candidiasis (Figure 3), any of which can affect the health-related quality of life. These features of xerostomia can lead to the inability of the patient to take necessary medications and can influence intake of proper nutrients, leading to malnutrition and a decline in overall health.
There are multiple causes of xerostomia attributable to various mechanisms. For example, anticholinergic effects of many medications, alcohol and drug abuse, and damaging head and neck radiation can cause xerostomia. There are many comorbidities from HIV such as cardiac disease, diabetes, and mental health disorders that occur in people with HIV. As a result, many of the medications especially antidepressants, anxiolytics, diuretics, and antihistamines being taken for these comorbidities lead to xerostomia.
There are still differing studies of the xerostomic effects of ARV medications used to treat HIV. Antiretroviral drugs are now recommended for all patients with an HIV diagnosis regardless of their immune system status, as ART enables the immune system and works to decrease the possibility of HIV transmission from one person to another.
There are currently six classes of drugs used to treat HIV infection: nucleoside reverse transcriptase inhibitors (NRTIs), nonnucleoside reverse transcriptase inhibitors (NNRTIs), protease inhibitors (PIs), integrase inhibitors (INSTIs), fusion inhibitors (FIs), and chemokine receptor antagonists (CCR5 antagonists). In most cases, combination therapy includes three drugs to reduce HIV viremia to below detectable levels. A review of current literature suggests a relationship between orofacial adverse reactions related to these drug classes. In particular, both NRTIs and PIs are associated with the most significant oral side effects of xerostomia. However, recent studies indicate HIV-positive patients who are not on ART are more vulnerable to decreased salivary flow rates.[10] In one study, ART did not affect xerostomia or salivary flow rates in the studied population group. Whereas low CD4 counts (<200cells/µL) have been attributed by many authors to being a significant risk factor for xerostomia and hyposalivation, others did not find this correlation significant.[11],[12]
More significant in the era of ART is the increased prevalence of salivary gland disease. Salivary gland disease can arise in 4-8% of adults and children with HIV.[13] HIV salivary gland disease (HIV-SGD) is a distinct disorder characterized by persistent major salivary gland swelling and xerostomia. HIV-SGD most commonly affects one or both parotid glands, sometimes without xerostomia. In some cases, salivary gland enlargement may be the first clinical manifestation of HIV infection, but more often it is a sign of late HIV infection.[13] The exact pathophysiology of HIV-SGD is unknown, but its origins include lymphoepithelial lesions, cysts, intraglandular lymph nodes, and an inflammatory infiltrate similar to what is often observed in Sjögren syndrome, although with distinct histopathologic and serological differences. In the infiltrate, there are persistent circulating CD8+ lymphocytosis and diffuse visceral CD8+ lymphocytic infiltration.[14]
Inflammatory or infectious diseases are the second most common group of salivary gland disorders in HIV disease, followed by neoplastic lesions. Kaposi sarcoma can account for 10% of malignant salivary gland neoplasms in HIV disease.[15]
Treatment of salivary gland enlargement in HIV remains nonspecific but could include aspiration of cystic lesions, superficial parotidectomy to alleviate swelling, and external radiation therapy for benign parotid hypertrophy.
Reports of xerostomia in people with HIV must be given careful consideration as the xerostomia most often reflects an adverse effect of ART and/or HIV salivary gland disease.[16] Patients must be advised of the risks of caries and gingival inflammation as well as the physiological effects of xerostomia. The goal for the patient is to alleviate the symptoms by increasing the intake of water, sugar-free gum or candies, salivary substitutes, or therapeutic management with cholinergic agents. Overlying these treatments must be careful monitoring of oral hygiene and the use of prescription topical fluorides.
Figure 1 Figure 2 Figure 3

[1] Centers for Disease Control and Prevention. HIV in the United States: At a Glance.
[2] Centers for Disease Control and Prevention. Florida--State Health Profile. 2015.
[3] Sweeny D. New HIV cases soar in Florida. South Florida Sun-Sentinel. July 24, 2015.
[4] Florida Department of Health. HIV Cases. FLHealthCharts.com.
[5] Greenspan D, Komaroff E, Redford M, et al. Oral mucosal lesions and HIV viral load in the Women's Interagency HIV Study (WIHS). J Acquir Immune Defic Syndr. 2000 Sep 1;25(1):44-50.
[6] Nokta M. Oral manifestations associated with HIV infection. Curr HIV/AIDS Rep. 2008 Feb;5(1):5-12.
[7] Porter SR, Scully C. HIV topic update: protease inhibitor therapy and oral health care. Oral Dis. 1998 Sep;4(3):159-63.
[8] Ceballos-Salobreña A, Gaitán-Cepada L, Ceballos-Garcia, et al. Oral lesions in HIV/AIDS patients undergoing highly active antiretroviral treatment including protease inhibitors: a new face of oral AIDS? AIDS Patient Care STD. 2000 Dec;14(12):627-35.
[9] Busato I, Tomaz M, Toda A, et al. Prevalence and impact of xerostomia on the quality of life of people living with HIV/AIDS from Brazil. Wiley Online Library, November 5, 2012.
[10] Cherian, Jeftha A. Xerostomia and salivary flow rates in HIV patients. South African Journal of Dentistry. vol.72, n.2, p.62-67. March 2017.
[11] Navazesh M, Mulligan R, Barrón Y, et al. A 4-year longitudinal evaluation of xerostomia and salivary gland hypofunction in the Women's Interagency HIV Study participants. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003 Jun;95(6):693-8.
[12] Nittayananta W, Talungchit S, Jaruratanasirikul S, et al. Effects of long-term use of HAART on oral health status of HIV-infected subjects. J Oral Pathol Med. 2010 May;39(5):397-406.
[13] Shetty K. Implications and management of xerostomia in the HIV-infected patient. HIV Clinician. March 2005.
[14] Mandel L, Kim D, Uy C. Parotid gland swelling in HIV diffuse infiltrative CD8 lymphocytosis syndrome. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998 May;85(5):565-8.
[15] Chieng DC, Argosino R, McKenny BJ, et al. Utility of fine-needle aspiration in the diagnosis of salivary gland lesions in patients infected with human immunodeficiency virus. Diagn Cytopathol. 1999 Oct;21(4):260-4.
[16] Panayiotakopoulos GD, Aroni K, Kyriaki D, et al. Paucity of Sjogren-like syndrome in a cohort of HIV-1-positive patients in the HAART era. Part II. Rheumatology (Oxford). 2003 Oct;42(10):1164-7.

